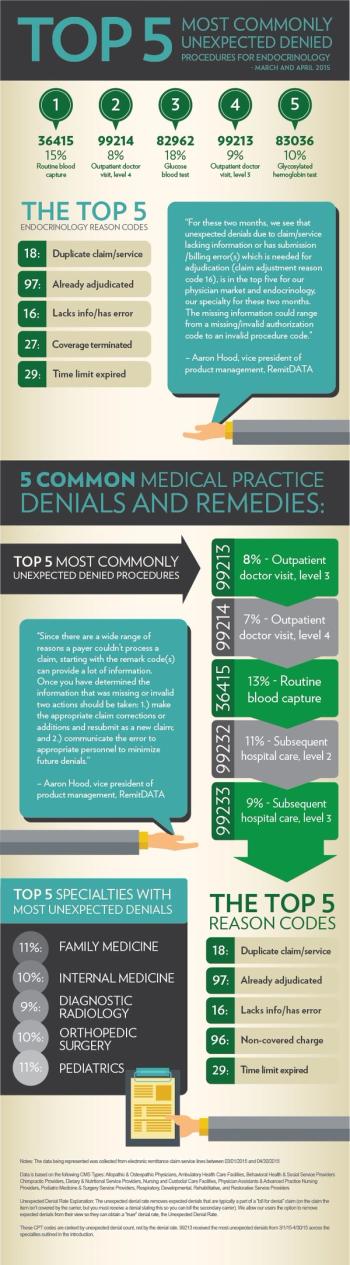
Get insight on the most common unexpected denials at practices nationwide, with a special focus on endocrinology, from RemitDATA.

Get insight on the most common unexpected denials at practices nationwide, with a special focus on endocrinology, from RemitDATA.

ICD-10 Charts is a free tool to aid the coding transition, but also a gift from a son to his internist father to keep his private medical practice alive.

Make sure your practice is getting paid what it is owed for the work you perform with these four tips.

Thinking about outsourcing your medical billing? Here are nine questions to ask a prospective outside biller or billing service.

Before deciding to provide and bill for chronic care management, a practice should make sure it has the necessary staff and support structures first.

As Oct. 1 approaches, get your physicians ready by determining how much and what kind of ICD-10 training they'll need.

Answers from our coding expert on questions regarding benchmarking resources; 92225 vs. 92226; procedures in visit notes; and chronic care management.

Coverage and reporting requirements for pneumococcal vaccine in Medicare beneficiaries has recently changed. Here's what you need to know.

Reduce the number of unpleasant surprises when the ICD-10 coding system goes live in October by starting tests now.

As we get closer to the ICD-10 transition, medical billers are likely finding some familiar symptoms among the new code set.

The ICD-10 coding system goes into effect October 1, but you may not be totally finished with the old codes for several weeks.

RemitDATA's Aaron Hood explores the most common unexpected denials at practices nationwide, with a special focus on radiology.

ICD-10 will be here before you know it. Here's what you need to do before October 1.

Make sure your practice is ready for changes in documentation analysis and quality reporting tied to the ICD-10 coding transition.

The changes in the new ICD-10 coding system will help you do your job better. Here are some changes you'll be happy to meet.

Answers from our coding expert on questions regarding Level 4 documentation and RN reimbursement.

It's possible to be reimbursed for a preventive visit and a problem-focused visit performed on the same day, but proper documentation and coding is critical.

Think coding is hard now? ICD-10 will require far greater specificity and documentation. Here are two ways to start preparing.

You can boost your payment stream significantly by using rejected claims as a learning opportunity. Here's how.

If you're looking to combat rising business costs at your medical practice your best bet is effective coding. Here's how to get started.
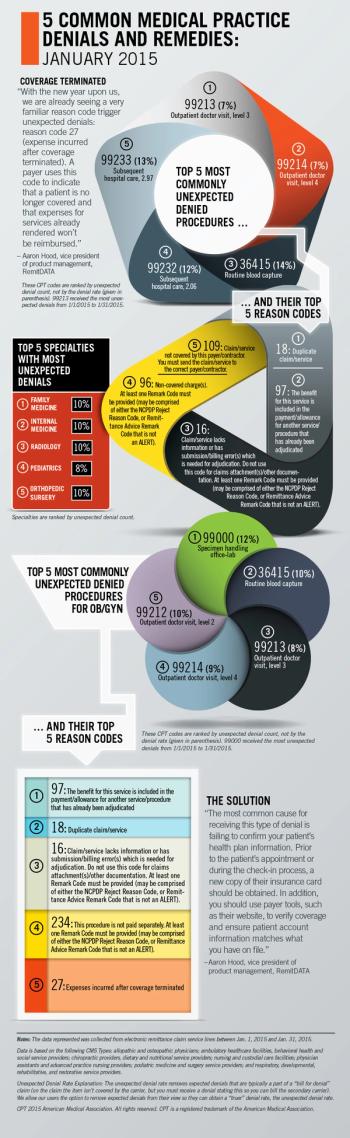
RemitDATA's Aaron Hood explores the most common unexpected denials at practices nationwide, with a special focus on OB/GYN.

ICD-10 training for your staff will vary by learning style and practice role. Here are eight resources to meet your needs.

An important part of ICD-10 readiness is ensuring all hardware and software is evaluated via a systems inventory.

Medicare's value-based modifier is a new fee schedule adjustment that will reward or penalize physicians for quality of care in 2015.

Answers from our coding expert on questions regarding discharge code requirements; complex care coordination; and counseling code confusion.